Blog Post
The COVID-19 pandemic was used as an excuse to murder elderly and disabled people
By Jonathon Van Maren
The COVID-19 pandemic has exposed many things about our society over the past several months.
In Canada, it highlighted the appalling conditions of many of the nursing homes where we warehouse the elderly. The military had to be sent in when those tasked with their care abandoned them in their beds, and soldiers described finding elderly men and women lying in their own filth and crying for help and rooms infested by ants and cockroaches. Over 80% of Canada’s COVID-19 death toll was among elderly people.
The same was true in New York, where COVID-19 patients were put in nursing homes by order of Governor Cuomo. The virus raced through the homes “like a fire through dry grass,” killing the elderly residents.
In Sweden, the pandemic was used as an excuse to eliminate elderly people. I wish that were an exaggeration. From Wesley Smith in National Review:
The health authorities have received many complaints about how elderly relatives were treated. A consistent theme is that nursing home residents with suspected Covid-19 were immediately placed on palliative care and given morphine and denied supplementary oxygen and intravenous fluids and nutrition. For many this was effectively a death sentence.
“People suffocated, it was horrible to watch. One patient asked me what I was giving him when I gave him the morphine injection, and I lied to him,” said Latifa Löfvenberg, a nurse. “Many died before their time. It was very, very difficult.”
The problem seems to have been the guidelines issued by the National Board of Health and Welfare. At the start of the pandemic it suggested that doctors triage patients according to their so-called biological age, weighing overall health and the prospects for recovery, before making treatment decisions…
The idea was to keep hospital ICUs from being overwhelmed by older patients with a low chance of survival. However, the surge never happened. Instead, the elderly were denied access to unused facilities. “These guidelines have too often resulted in older patients being denied treatment, even when hospitals were operating below capacity,” according to critics who spoke to the WSJ. “Occupancy in the country’s intensive-care units, for instance, has yet to exceed 80%, according to government officials.”
That devolved into active killing: Yngve Gustafsson, a geriatrics specialist at Umea University, told the BMJ that the proportion of older people in respiratory care nationally was lower than at the same time a year before, even though people over 70 were the worst affected by Covid-19. He, too, was aghast at the practice of doctors prescribing a “palliative cocktail” for sick older people in care homes over the telephone.
“Older people are routinely being given morphine and midazolam, which are respiratory-inhibiting,” he told the Svenska Dagbladet newspaper, “It’s active euthanasia, to say the least.”
And then there was this story out of Texas:
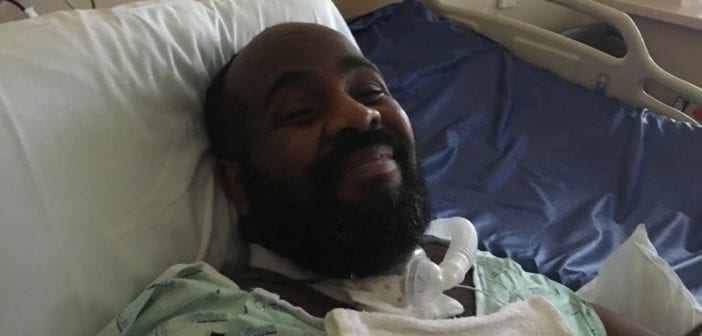
Michael Hickson, a 46-year-old COVID-19 patient, was starved and left without adequate treatment for his illnesses at St. David’s South Austin Medical Center. His wife, Melissa, says the hospital refused to treat his illnesses because of his disability.
Michael Hickson became quadriplegic due to receiving CPR after he went into sudden cardiac arrest while driving Melissa to work in May 2017. Melissa and their five children stayed by Michael’s side throughout his recovery. He landed back in the hospital in 2020 after contracting COVID-19 and pneumonia from a staff member at his nursing home.
Michael was conscious and alert but could not communicate verbally. He responded to jokes, shook his head, and puckered his lips on a FaceTime call when Melissa requested a kiss. Melissa asked if she could pray with her husband and their children, to which he nodded “yes.” But the doctor soon told Melissa her husband would be placed in hospice against her will. In a recorded conversation, the St. David’s doctor told Melissa her husband would not receive treatment because of his disability, despite her wishes.
St. David’s doctor: “So as of right now, his quality of life – he doesn’t have much of one.”
Melissa: “What do you mean? Because he’s paralyzed with a brain injury he doesn’t have quality of life?”
St. David’s doctor: “Correct.”
While Michael’s wife and another family member were litigating in court who would be Michael’s permanent guardian, a judge named an Austin-area organization called Family Eldercare as temporary guardian over Michael. Family Eldercare granted the doctor’s orders to not treat Michael and instead place him in hospice. Alarmingly, the doctor reiterated the scary reality that she had zero say in whether her husband lived or died. The doctor told Melissa, “but at this point, we are going to do what we feel is best for him along with the state and this is what we decided… this is the decision between the medical community and the state.”
Michael was left without food or treatment for six days despite Melissa’s will to save her husband. He passed away from the untreated illnesses on June 11, 2020.
Now, Melissa and her children grieve their beloved husband and dad. Melissa stated, “I’m struggling to understand how and why this could ever happen. I lost my best friend, my better half, the other half of my heart.” She continued:
I was stripped of my rights as a wife, and left helplessly watching my husband be executed. I now have no husband, a widow at 47. My children left with no father to celebrate Father’s Day. All taken away from us. I have no other words to express how I feel today except hurt, angry, and frustrated.
In times of crisis, we often discover who we really are. In times of panic and uncertainty, we learn much about what—and who—we really value. The COVID-19 pandemic has taught us something about how our society now views the elderly and the disabled, and we should be very, very ashamed.






Never thought it would ever happen in America. This is straight out of the Nazi and Marxist handbook Vote wisely in Nov.
By which I assume you mean vote Democrat?
“Republicans control all statewide Texas offices, both houses of the state legislature and have a majority in the Texas congressional delegation.”
“Gregory Wayne Abbott is an American attorney who has served as the 48th governor of Texas since January 20, 2015. A member of the Republican Party, Abbott previously served as the 50th attorney general of Texas from 2002 to 2015.”
Judge Guy Herman, the judge in this case, is a Democrat. That said, that is only part of the problem. The ethics of the doctor and the court appointed guardians are also an issue.
Just to be clear: the political affiliation of the judge impartially applying the laws as crafted and protected by the legislators is an issue to you?
don’t be so alarmed dear Christina. In my opinion, a country which is willing to heartlessly kill her unborn future is able to do everything else to practically any other citizen. let’s pray for repentence. our small country Malta, although with no natural resources and the most overpopulated in Europe takes care of its vulnerable both young and old and to avoid deaths we all went to drastic measures during this pandemic with only nine deaths which could not be avoided. At present we have only 15 active cases known. we need to pray for repentence